
Obesity left untreated can cause serious health problems over time. You can take action today. Discover your options.

Obesity left untreated can cause serious health problems over time. You can take action today. Discover your options.
Sleeve gastrectomy is now the most common operation performed for obesity in Australia.
The normal stomach holds about 1.5 litres of food. We reduce the size of the stomach by resecting a large part of the stomach.
The resected part of the stomach is removed completely. The remaining “sleeve” of stomach holds only about 150-250mL.
The effect of the sleeve gastrectomy is that you can eat a very small meal, feel full and satisfied, and the hunger you would currently feel after eating such a small meal does not occur.
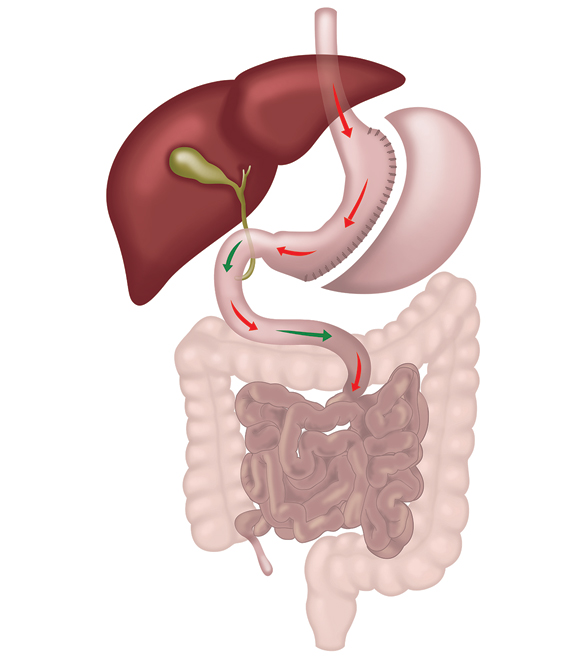
The effect of the sleeve gastrectomy is that you can eat a very small meal, feel full and satisfied and the hunger you would currently feel after eating such a small meal does not occur.
When assessing the risks of surgery you must also consider and balance the risks of not having the surgery and remaining significantly overweight which can include an increased risk of heart disease, diabetes, stroke and some cancers.
Our sleeve gastrectomy surgeries are performed only in Private Hospitals. The costs of surgery can vary according to your particular private health cover and Medicare rebates. It may be possible to fund out of pocket costs from your Superannuation.
We now also offer a uninsured option for selected patients having a Sleeve Gastrectomy.
When we remove the stomach we use a stapling device to seal the stomach. A triple row of titanium staples seals the cut edges of the stomach. This produces a very secure closure of the cut edges of the stomach. However, right at the top edge of the stomach there can be a failure of the staples to seal fully. If this happens there will be a leakage of stomach contents into the abdominal cavity. This usually only occurs in the first 2 weeks after the operation and occurs in about 1% of patients. If you have had previous stomach surgery such as a gastric band the leak rate is significantly higher and must be discussed thoroughly with your surgeon.
This is a very serious complication and could keep you in hospital for several weeks. Further operation may be required which may not be laparoscopic (keyhole) surgery.
The leak will eventually seal by itself or by other treatments and once this occurs the operation will work just as well as if the complication had not occurred.
On rare occasions part of the sleeve will narrow and you may be unable to swallow foods properly. This is easily fixed, in most cases, by a simple gastroscopy and opening up of the narrowed area using an inflatable balloon. In very rare cases it may not be possible to cure the problem and conversion to a gastric bypass may be necessary.
This is uncommon and mostly seen at the upper end of the sleeve. Our preferred option in this situation is to convert to a gastric bypass.
Most patients will have some reflux in the first few months after a sleeve gastrectomy which may be controlled with acid lowering medications. A very small group of patients may experience very severe reflux which cannot be controlled by medication. In this instance conversion to a gastric bypass may be necessary.
Unfortunately, a small number of patients will either not lose the expected amount of weight or will, at a later date, put some of the weight back on. We have a comprehensive multi-disciplinary service that can help you get back on track.
Following Sleeve Gastrectomy surgery, each patient has the potential of vitamin deficiency. LapSurgery Australia strongly recommends to all patients that they take regular, daily multivitamins in order to reduce the risks of other medical conditions such as osteoporosis, thiamine deficiency and other vitamin and mineral deficiencies. More information about vitamins is given to patients at the time of consultation with our dietitian.
Learn more about Sleeve Gastrectomy surgery here.
The following are the most common of the complications but please note that this is not a comprehensive list of possible complications but does cover most events.
Anaesthetic risks are extremely low because when you come to your operation any conditions which might increase your anaesthetic risk such as high blood pressure, diabetes or sleep apnoea will have been brought under control. All of our anaesthetists are experienced with dealing with the specific problems of patients with excess weight and have full access to all of the tests and information gathered during your preoperative assessment.
Although uncommon, bleeding can occur during an otherwise routine operation and could require blood transfusion and possibly abandoning the laparoscopic (keyhole) approach for a major incision in the abdomen. Occasionally bleeding can commence some hours after an operation and require a return to the operating theatre.
Again these are uncommon with laparoscopic surgery, but occasionally one of the small keyhole wounds can become infected and require antibiotics or drainage. Uncommonly, an infection inside the abdominal cavity or the chest can occur.
Although uncommon, during laparoscopic surgery it is possible to inadvertently damage another organ such as the spleen or the bowel. Normally this can be diagnosed and repaired during the operation but very rarely this damage may not be obvious until some hours or even days after the procedure and will then require appropriate management.
Rarely, it is not possible to complete an operation with keyhole surgery and a full abdominal incision may be necessary. This is more likely to be the case if you have had previous surgery on your stomach such as a gastric band or stomach stapling.
Blood clots to the legs or the lungs are a very serious complication. At LapSurgery we use the maximum protection against this occurring. Shortly before the operation you will be given a blood thinning injection and have stockings placed on your legs. A further device will also be placed on your legs which keeps pumping blood through your legs while you’re asleep to minimise the chance of a clot forming whilst you are on the operating table.
Using these precautions and the early mobilisation after the surgery that is possible with the keyhole operation, these complications have been uncommon in our patients.
Our experienced surgeons can discuss the Sleeve Gastrectomy or other weight loss surgery with you at our Dandenong North, Berwick, Frankston, Warragul or Cranbourne locations.
See addresses for our locations here.
At LapSurgery, long before your operation takes place, you will undergo a comprehensive assessment of your health so that we can identify any risks and minimise these.
If, after your initial visit to the surgeon, you decide to go ahead with surgery we will arrange a comprehensive set of blood tests and an appointment with a specialist physician experienced in preparing patients for surgery and minimising any risks. Patients with severe obesity will often have other conditions related to their weight (comorbidities) which, in many cases, can increase the risks of surgery. Poorly treated high blood pressure, poorly controlled diabetes, untreated sleep apnoea, vitamin deficiencies, urine infections and cardiac problems are often present and these must be treated properly before surgery. Sometimes this will involve other tests such as sleep tests, blood pressure monitoring and heart tests before we can go ahead with the surgery. The very high safety levels with which we perform this sort of surgery are very dependent on this initial thorough investigation and optimisation of treatment of comorbidities before surgery takes place.
One of the risks of this sort of surgery, often not listed in the usual complications, is the lack of education and understanding of both the pre-operative preparation and the post-operative management of your lifestyle and dietary habits. We have a dietitian at LapSurgery to educate and supervise your weight loss journey. We are also very aware that years of frustration with your weight problems, and some of the prejudice you will have faced about your weight, can have an effect on your mental well-being and so all patients are seen initially by our psychologist as part of the assessment. Follow up counselling is available should you wish.
Prior to surgery we require the following appointments:
You will also have the following:
Our surgery package after Sleeve Gastrectomy (Gastric Sleeve) Surgery also includes:
We also offer an “uninsured” option to selected patients for sleeve gastrectomy surgery, without private health insurance covering bariatric surgery. We are committed to providing comprehensive, best practice, high quality care to our patients. That’s why our package price includes cover for return visits to hospital (for specific surgery related problems) within 28 days of your surgery, giving you unparalleled peace of mind. The uninsured package has all of our usual inclusions like consultations with your surgeon, physician, psychologist, dietitian and exercise professional. See our pricing for private health insurance or uninsured options here.
*Uninsured option is available only for some patients for sleeve gastrectomy surgery, in specific hospitals. Please contact us to find out if you qualify.
What you have read above is a summary of the operation of sleeve gastrectomy. This is not sufficient information in itself and every aspect of the surgery, the preparation and the possible complications are always specific to an individual and must be discussed at length with your surgeon.
Good results are only achieved when you, the patient, are well informed and educated about the procedure and the operation is done by a dedicated, experienced multidisciplinary team such as we provide at LapSurgery.
We’ve created a series of videos to explain details about the weight loss surgery process.
The team at LapSurgery Australia are recognised for their exceptional and major contribution to the Government sponsored Bariatric Safety Registry (BSR). The BSR tracks surgical complications and provides an unbiased safety record for weight loss surgery.