Laparoscopic Gastric Bypass
Summary:
- Experienced, senior team providing a multidisciplinary approach to surgery.
- Price: $10,000-13,000 for patients with Private Health Insurance covering weight loss surgery
Gastric Bypass Surgery
Laparoscopic (keyhole) gastric bypass is a well established obesity surgery which creates a smaller stomach and bypasses part of the small intestine, reducing the absorption of food. At LapSurgery we have been performing this procedure since 2009. It is particularly effective for patients with Type 2 diabetes.
There are several slightly different ways of performing a gastric bypass, at LapSurgery Australia we perform the most commonly used version referred to as a Roux-en-Y gastric bypass. Whilst it is a more complex operation than the sleeve gastrectomy or the gastric band, it can be performed with keyhole surgery.
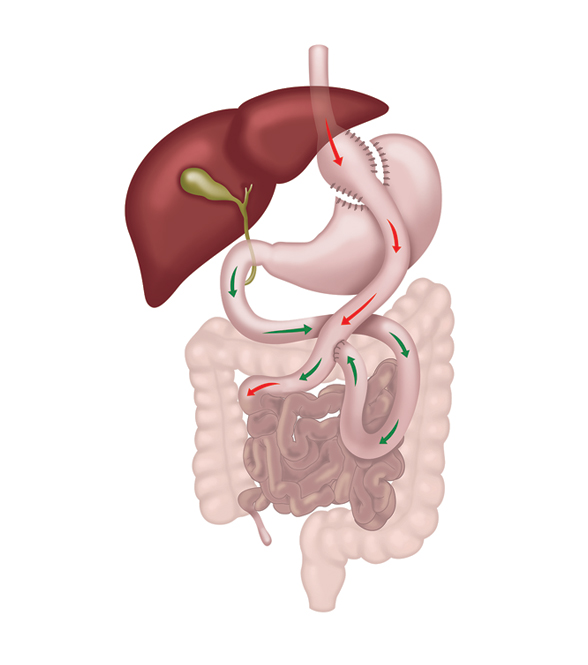
- Gastric bypass surgery has been performed for over 30 years and its effectiveness is well proven
- Gastric bypass surgery is now usually performed with keyhole surgery
- Complication rates are very low
- Patients commonly lose 60 to 70% of their excess weight over 18 to 24 months
- Patients with type II diabetes experience improvement in diabetes control, often within days of the operation
- Many patients with Type II diabetes can achieve long-term remission
- Associated conditions such as high blood pressure and sleep apnoea often improve quickly after surgery
- Hospital stay is 3 to 4 days when performed with laparoscopic (keyhole) surgery
- Patients can be back at work in as little as two to three weeks depending on the job
- You will be able to eat (small amounts of) most food types
- Long-term follow-up, as in all bariatric operations, is vital.
At LapSurgery Australia we perform each of the major types of weight loss surgery. In most cases we do not recommend the gastric banding so the choice lies between the sleeve gastrectomy and the gastric bypass. Studies comparing the two over five-year time frames show very similar degrees of weight loss.
However, patients with Type II diabetes and those with gastric reflux have better results with the gastric bypass. The choice of operation will be discussed with you very thoroughly, and in the end, we present the facts and you make the decision as to which form of surgery suits you best.
The gastric bypass works in four different ways:
1. Suppression of hunger
After Gastric Bypass surgery, food coming down the oesophagus enters the small stomach remnant pouch. Food sits in this part of the stomach for a few minutes and stimulates the nerve endings in the top of the stomach. These nerve endings are there to tell the brain when the stomach is physically full. Of course, the stomach is nowhere near full but the brain doesn't know that! Appetite is then turned off and this reduction of hunger is what makes it possible to eat much less food without the strong hunger that you get when you go on a strict diet.
2. Limited portion sizes
As the capacity of the upper part of the stomach is much less you simply can't get a lot down! But don't worry; you can eat enough to stay healthy. Food passes reasonably quickly into the small bowel so as long as you eat slowly, enjoy your food and don't rush you should have no problems.
3. Some of the food you eat will not be absorbed by your body
After food exits the small upper stomach it travels along the small bowel for about 1½ metres before it joins with the bypassed part of the small bowel. So in the one and a half metres of this limb there is food but fewer digestive enzymes. Food can't be absorbed without digestive enzymes. So it's not until around 2 metres along the small bowel until there is both food and digestive enzymes so that absorption can take place. That means that 2 metres or so of your small bowel no longer absorbs food.
When comparing costs, please be aware that our costs include all of the following:
- Initial consultation with Surgeon
- Pre-operative assessment with Specialist Physician
- Clinical Psychologist consultation
- Dietitian consultations inclusive of 1x pre-operative, 3x post-operative appointments
- Exercise professional appointment
- Surgeon and Assistant Surgeon
- Access to on-call Surgeon at all times
- Comprehensive after care at Medicare rebate
Our operations are performed only in Private Hospitals. These costs can vary according to your particular private health cover. It may be possible to fund this out of pocket cost from your Superannuation.
See if you are eligible for the Gastric Bypass, and check out our quote generator here:
Calculate quoteAll surgery involves some risk. Risks can be broken down into two groups, those related to surgery in general and those specific to the operation being performed. Risks of surgery in general include risks of anaesthetics, infections inside the abdomen and in the wound, lung problems, blood clots in the leg or lungs and, very rarely, death. If you have other health problems such as heart or lung problems, diabetes, smoking the general risks of surgery are increased.
When assessing the risks of surgery you must also consider and balance the risks of not having the surgery and remaining significantly overweight
These will be discussed in detail with you prior to the operation by your surgeon.
Complications in the first couple of weeks
The major risk in the first two weeks is that the join of the small bowel to the stomach does not heal properly and gastric fluid leaks into the abdominal cavity causing peritonitis. This occurs in less than one in 100 operations in people who have not had previous gastric surgery. However, in people who have had a gastric band or a gastric stapling operation in the past the chance of a leak is higher and must be fully discussed with your surgeon before going ahead. Learn more about gastric bypass surgery here.
Should a leak occur, this is a very major complication which may well involve further surgery. This could include a major abdominal incision rather than keyhole surgery.
Hospital stay in this event could stretch into some weeks and involve a stay in the intensive care unit. Exactly how we deal with this complication can vary from person to person but, one way or another, the leak will seal and you should make a full recovery and still achieve very good results.
Complications occurring weeks, months or years after the operation
Narrowing of the join between the small bowel and the stomach.
Occasionally, the join between the upper part of the stomach and the small bowel can narrow down and cause difficulty swallowing. This is easily fixed with a gastroscopy and dilatation performed under sedation with only a couple of hours in the hospital. This usually only occurs in the first few weeks after the operation, not later on.
Dumping syndrome
Dumping syndrome is a possible side-effect of the gastric bypass surgery particularly in the first two or three months after the operation. Dumping syndrome is usually caused by eating a high fat or high sugar food. After eating, you may feel more mild symptoms like cold sweats or nausea or you may have a more severe reaction causing dizziness, diarrhoea or vomiting. The symptoms usually last a short time but you may experience symptoms of low blood sugar levels 1-3 hours after eating and need to eat a high carbohydrate food. If this is happening more than occasionally, keeping a food record and a visit to our dietitian should get things back to normal very quickly.
Internal Hernias
When we rearrange parts of the small bowel for the gastric bypass there are two places where we create a “hole” where part of the small bowel could get stuck. This can cause intermittent severe abdominal pain or even a complete blockage of the bowel. It is not always easy to diagnose and should always be considered if you have an episode of severe abdominal pain even some years after the operation. We are now very conscious of this possibility and part of every operation involves closing the two holes where the small bowel can get stuck. Even so there remains a small possibility that this could happen in the future. Surgery would probably be required and may not be able to be done with keyhole surgery. The chance of this happening is less than 5% for the rest of your life.
Ulcer at the join of the small bowel and the stomach pouch (Anastomotic Ulcer)
This is an uncommon condition and usually can be fixed with acid reducing tablets and some variation to diet.
Weight gain
Unfortunately, a small number of patients will either not lose the expected amount of weight or will, at a later date, put some of the weight back on. It is vital that you understand that the bypass is a tool to help keep your weight down. It is not a procedure which can protect you forever from gaining weight. You must realise that you have a genetic predisposition to weight gain and that long-term attention to the principles of healthy diet, exercise and lifestyle are essential to maintain your weight loss results. Long-term follow-up, which we provide at LapSurgery Australia, is absolutely essential to your long-term success. If there you see any significant weight gain you must see us immediately so that we can help you. Unfortunately, some people feel they have failed if their weight starts to increase and feel too embarrassed to come back and see us. The more weight you put on before seeking help, the more difficult it will be to reverse. We will never make you feel embarrassed about any weight gain; we are here to help you.
Vitamin deficiency
Following weight loss surgery each patient has the potential of vitamin deficiency and so LapSurgery Australia recommend to all patients that they take daily multivitamins in order to reduce the risks of other medical conditions such as osteoporosis, thiamine deficiency and other conditions. More information is given to patients at the time of consultation.
Our experienced surgeons can discuss the Gastric Bypass or other weight loss surgery with you at our Dandenong North, Berwick, Frankston, Warragul or Cranbourne locations.
See our location addresses here.
The following are the commonest of the complications but please note that this is not a comprehensive list of possible complications but does cover most events.
The Risk of the Anaesthetic
Anaesthetic risks are extremely low because when you come to your operation any conditions which might increase your anaesthetic risk such as high blood pressure, diabetes or sleep apnoea will have been brought under control. All of our anaesthetists are experienced with dealing with the specific problems of patients with excess weight and have full access to all of the tests and information gathered during your preoperative assessment.
Bleeding
Although uncommon, bleeding can occur during an otherwise routine operation and could require blood transfusion and possibly abandoning the laparoscopic (keyhole) approach for a major incision in the abdomen. Occasionally, after a routine operation, bleeding can commence some hours after an operation and require a return to the operating theatre.
Infections
Again these are uncommon with laparoscopic surgery, but occasionally one of the small keyhole wounds can become infected and require antibiotics or drainage. Uncommonly, an infection inside the abdominal cavity or the chest can occur.
Damage to Other Organs
Although uncommon, during laparoscopic surgery it is possible to inadvertently damage another organ such as the spleen or the bowel. Normally this can be diagnosed and repaired during the operation but very rarely this damage may not be obvious until some hours or even days after the procedure and will then require appropriate management.
Conversion to Open Operation
Rarely, it is not possible to complete an operation with keyhole surgery and a full abdominal incision may be necessary. This is more likely to be the case if you have had previous surgery on your stomach such as a gastric band or stomach stapling.
Blood Clots to the Legs or Lung (Pulmonary Embolus)
Blood clots to the legs or the lungs are a very serious complication. At LapSurgery we use the maximum protection against this occurring. Shortly before the operation you will be given a blood thinning injection and have stockings placed on your legs. A further device will also be placed on your legs which keeps pumping blood through your legs whilst you're asleep to minimise the chance of a clot forming whilst you are on the operating table.
Using these precautions and the early mobilisation after the surgery that is possible with the keyhole operation, these complications have been uncommon in our patients.
What you have read above is a summary of Roux-en-Y Gastric Bypass Surgery. This is not sufficient information in itself and every aspect of the bypass, including the preparation for surgery and the possible complications, is always specific to an individual and must be discussed at length with your surgeon.

The team at LAPSurgery Australia are recognised for their exceptional and major contribution to the Government sponsored Bariatric Safety Registry (BSR). The BSR tracks surgical complications and provides an unbiased safety record for weight loss surgery.
Video Hub
We've created a series of videos to explain details about the weight loss surgery process.
From Appointment to Assessment
1minMarilyn's Story
2minAre you a candidate?
Use our BMI calculator to check your eligibility and get a price estimate.